Obtain good stability with good pin spread:Īppropriate pin fixation with good pin spread is necessary to achieve stability. The anterior structures of the elbow will be draped over the distal edge of the distal humeral metaphysis.ģ. If the pulse does not return after closed reduction but the hand remains well perfused, inpatient observation for 24-48 hours is necessary to monitor for compartment syndrome.9,10įigure 3: A curvilinear incision over the antecubital fossa creates good exposure for evaluation of neurovascular injury. In the case of a pink (perfused) pulseless hand, CRPP can be attempted on an urgent, rather than emergent, basis. If perfusion is not returned, anterior exploration is necessary to investigate arterial injury entrapment in the fracture. This can be done through a 4-5 cm transverse anterior incision in the antecubital flexion crease.8 (Figure 3) If the hand remains cold and pale, emergent operative intervention is necessary. Closed reduction and percutaneous pin fixation is performed. Gentle traction and splinting in 30-45 degrees of flexion can sometimes restore perfusion by decreasing the tension on the anterior neurovascular structures.8 If this restores perfusion, urgent operative intervention is still necessary. In children, signs of compartment syndrome are typically increasing anxiety and agitation as well as need for pain medication.6 When neuropraxia and nerve injuries are present, sensory deficits can mask compartment syndrome and very close observation is necessary. The majority of patients with concomitant nerve injuries can still be treated with closed reduction. However, they should be observed inpatient post-operatively to monitor for compartment syndrome.7Ī pale pulseless hand needs emergent intervention. Capillary refill should be compared to the uninjured side. Antecubital ecchymosis and skin puckering raise concern for possible underlying neurovascular injury. Compartments should be palpated. Hand temperature, color, swelling, and digital turgor are important indicators of perfusion. If the radial pulse is absent, it is essential to carefully evaluate the perfusion of the hand. 
Vascular injury has been reported in up to 38% and nerve injury in up to 49% of patients with displaced type III supracondylar humerus fractures.5 From a vascular standpoint, palpation of the radial artery is important. Neurovascular exam can be difficult to elicit in an anxious and hurting child but is essential in the decision making process. 
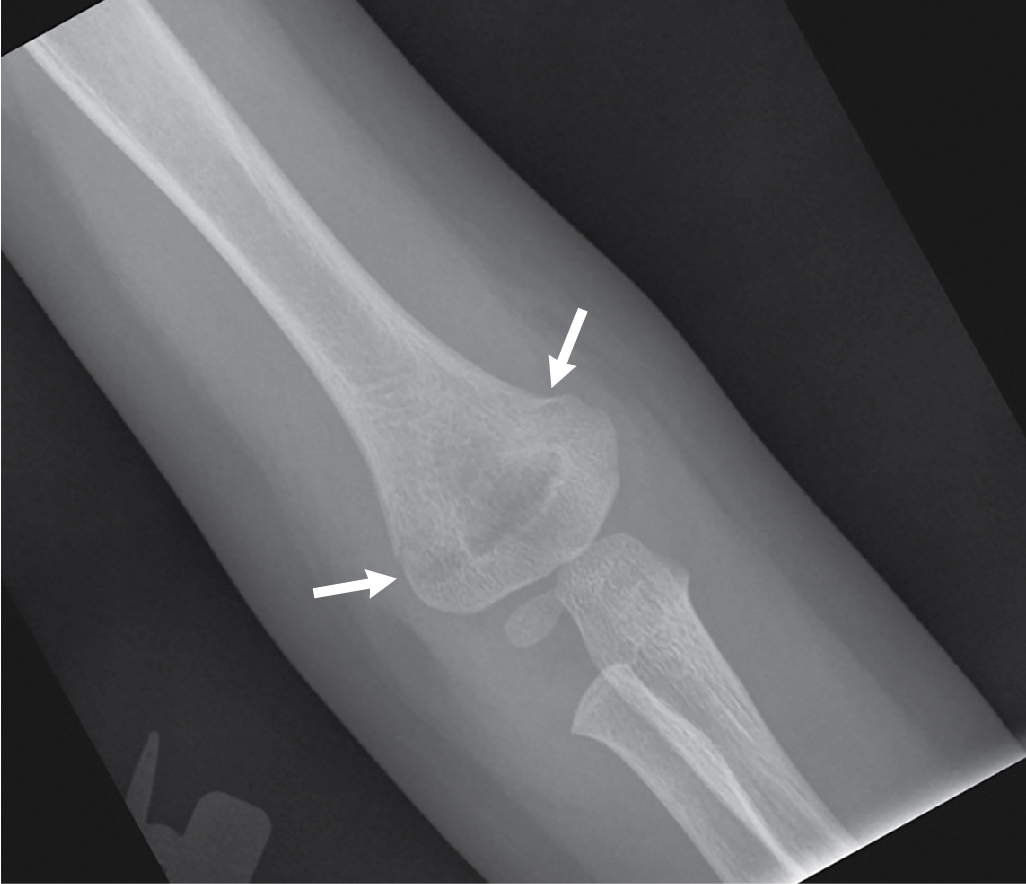
Document a good neurovascular exam and know when to act emergently. The image on the left shows the injured left elbow with medial comminution that has resulted in varus deformity.Ģ. The image on the left shows the uninjured contralateral right elbow with a normal Bauman’s angle. Normal angles were reported by Baumann to be between 75 and 80 degrees.2 A subsequent study showed the average Baumann’s angle to be 72 degrees, with a standard deviation of 4 degrees and a 95% confidence interval in normal elbows between 64 and 81 degrees.3 Rotation of the elbow, however, can have an impact on measurements.4 If in doubt of coronal plane deformity, radiographs of the uninjured contralateral elbow can be obtained for comparison.įigure 1: Medial comminution will result in varus deformity if not treated appropriatelyįigure 2: Bauman’s angle is measured by a line down the center of the humeral shaft and a line tangential to the capitellum. Carefully analyze your AP radiograph, looking for medial column comminution that will result in ultimate varus deformity. (See figure 1) This can be subtle in Gartland type II fractures and is easy to overlook if focused solely on the extension deformity.īauman’s angle can be used to help assess for coronal plane deformity.1 Bauman’s angle is measured by a line down the center of the humeral shaft and a line tangential to the capitellum (See Figure 2). Supracondylar humerus fractures can be more than just a sagittal plane issue. Varus deformity can be easy to miss at the time of injury in type II fractures, when one is easily focused on the lateral radiograph. Lawing, MD, Shriner’s Healthcare for Children - Florida 5 Tips for Pinning a Supracondylar Humerus Fracture
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
